Pancreatic-CT-CBCT-SEG | Breath-hold CT and cone-beam CT images with expert manual organ-at-risk segmentations from radiation treatments of locally advanced pancreatic cancer
DOI: 10.7937/TCIA.ESHQ-4D90 | Data Citation Required | 3.4k Views | 4 Citations | Image Collection
| Location | Species | Subjects | Data Types | Cancer Types | Size | Status | Updated | |
|---|---|---|---|---|---|---|---|---|
| Pancreas | Human | 40 | CT, RTSTRUCT, RTDOSE, Other | Pancreatic Cancer | Image Analyses | Public, Complete | 2022/08/23 |
Summary
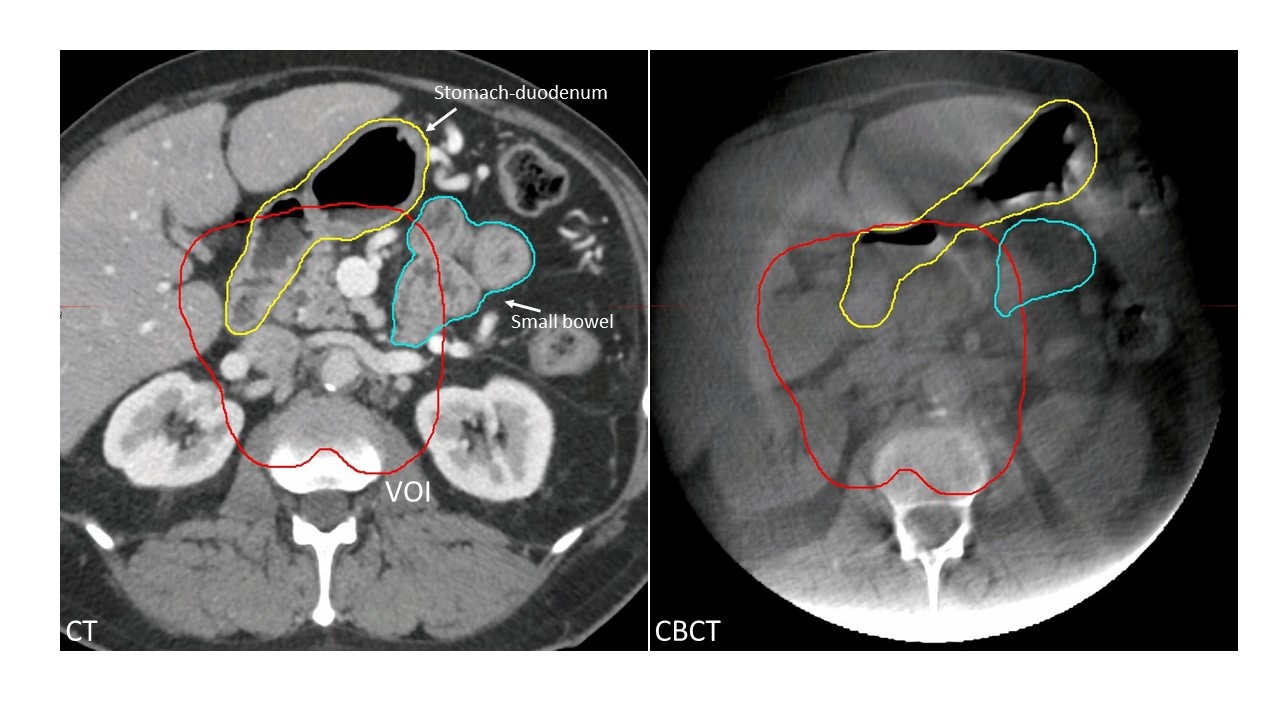
Accurate deformable registration between CT and cone-beam CT (CBCT) images of pancreatic cancer patients treated with high radiation doses is highly desirable for assessing changes in organ-at-risk (OAR) locations and shapes at treatment. The objective of this dataset is to provide a means of evaluating the performance of CT-to-CBCT deformable registration and auto-segmentation algorithms for delineating OARs. The data were retrospectively obtained with IRB approval from 40 patients who received ablative radiation therapy (>= 100Gy biologically effective dose) for locally advanced pancreatic cancer at Memorial Sloan Kettering Cancer Center. The images (one treatment planning CT and two CBCT scans from each patient) were acquired during a deep inspiration breath-hold verified with an external respiratory monitor. The planning CT was acquired with a diagnostic-quality scanner in helical mode with iodinated contrast. The kilovoltage CBCT scans were acquired without contrast and with the patient in the treatment position. Most of these (58 out of 80) were limited-view scans that were acquired with a 200-degree gantry rotation, resulting in faster acquisition and increased likelihood that the scan was acquired in a single breath hold. The limited-view CBCT scans had 25cm reconstructed diameter and 18cm length. The remaining 22 CBCT scans were acquired with 360-degree gantry rotation and were subsequently cropped to the same reconstructed dimensions as the limited-view scans. Each CBCT image was rigidly registered to the planning CT by aligning to an implanted fiducial marker or to a stent implanted during surgery. The CBCT was then resampled to match the voxel dimensions and volume of the planning CT. A volume of interest (VOI) was defined on the planning CT by expanding the microscopic-dose planning target volume by 1cm. Its purpose was to define a volume fully contained within both the planning CT and CBCT reconstruction volumes while excluding the periphery of the CBCT volume which was subject to cupping artifacts. It included the portions of the OARs receiving moderate to high dose. On the planning CT and each of the CBCT scans, two OAR volumes were delineated by a radiation oncologist: (1) stomach with the first two segments of duodenum, and (2) the remainder of the small bowel. On the CBCT scans, only the portions of the OARs within the VOI were delineated, whereas on the planning CT scans, the OAR delineations extended up to 2 cm outside of the VOI (in some cases contours may extend beyond these limits). The manual delineation was distributed among six radiation oncologists, such that the same physician completed all images belonging to the same patient. The contours were subsequently reviewed by two trained medical physicists and edited as needed to adhere to delineation guidelines. With this dataset researchers will be able to test the performance of deformable registration and auto-segmentation algorithms by comparison to physician-drawn OAR segmentations; an example can be found in a publication by Xu et al. Cone-beam CT scans of the pancreatic disease site are particularly challenging because of the presence of residual-motion-induced image artifacts such as blurring, streaking, x-ray scatter, as well as cupping artifacts from the limited-view acquisition. OAR structures in the CBCT often have limited visibility owing to the lack of contrast and the presence of gas pockets. Currently there is a lack of reliable CT-to-CBCT deformable image registration tools for soft tissues in abdomen. This dataset is unique from existing TCIA collections in that the context is focused on CBCT-guided radiation therapy of pancreatic cancer, the images are acquired with deep-inspiration breath-hold, and physician-drawn segmentations of organs at risk provide a criterion standard for testing registration and auto-segmentation algorithms.
Data Access
Version 2: Updated 2022/08/23
This change reflects an extension of the current dataset: the authors have added RT Dose files and original cone-beam CT images to the collection. The RT Dose consists of the dose distribution calculated on the planning CT and enables dosimetric analysis of the structures in the planning CT and in the resampled CBCT scans. The original CBCT images are those that were obtained in the clinical environment; as such they are useful for developing algorithms to be applied in the clinic. Ten of these original-format CBCT scans, from ten different patients (see the excel file provided with this version), are accompanied by RT Structure Sets containing repeat OAR delineations by two independent observers and contained within the VOI. The repeat delineations provide an informative way of seeing where two experts agree and disagree in the CBCT images.
| Title | Data Type | Format | Access Points | Subjects | License | Metadata | |||
|---|---|---|---|---|---|---|---|---|---|
| Images and Radiation Therapy Structures | CT, RTSTRUCT, RTDOSE | DICOM | Download requires NBIA Data Retriever |
40 | 40 | 370 | 24,246 | CC BY 4.0 | View |
| Reference RT to Planning CT table | Other | XLSX | CC BY 4.0 | — |
Additional Resources for this Dataset
The NCI Cancer Research Data Commons (CRDC) provides access to additional data and a cloud-based data science infrastructure that connects data sets with analytics tools to allow users to share, integrate, analyze, and visualize cancer research data.
- Imaging Data Commons (IDC) (Imaging Data)
Citations & Data Usage Policy
Data Citation Required: Users must abide by the TCIA Data Usage Policy and Restrictions. Attribution must include the following citation, including the Digital Object Identifier:
Data Citation |
|
|
Hong, J., Reyngold, M., Crane, C., Cuaron, J., Hajj, C., Mann, J., Zinovoy, M., Yorke, E., LoCastro, E., Apte, A. P., & Mageras, G. (2021). Breath-hold CT and cone-beam CT images with expert manual organ-at-risk segmentations from radiation treatments of locally advanced pancreatic cancer [Data set]. The Cancer Imaging Archive. https://doi.org/10.7937/TCIA.ESHQ-4D90 |
Detailed Description
Some notes about abbreviations in the dataset:
BSCB =“Bowel_sm” (i.e. small bowel) structure drawn on cone-beam CT
LL, LR = Lung left, Lung right
SDCB = Stomach-duodenum structure on cone-beam CT
SBPC = misspelled, should be BSPC which stands for Bowel Small in planning CT
SDPC = Stomach-duodenum on planning CT
BSPC = Bowel Small on planning CT
DIBH = “Deep inspiration breath hold”, may occur in the study description of the planning CT; will be explained in the text to users
“UNAPPROVED” = means that the contours were not approved for clinical use but they were checked by the research team.
Acknowledgements
We would like to acknowledge the individuals and institutions that have provided data for this collection. Supported in part by Award Number R21 CA223304 from the National Cancer Institute, National Institutes of Health, and by the MSK Cancer Center Support Grant/Core Grant P30 CA008748.
Related Publications
Publications by the Dataset Authors
The authors recommended the following as the best source of additional information about this dataset:
Publication Citation |
|
|
Han, X., Hong, J., Reyngold, M., Crane, C., Cuaron, J., Hajj, C., Mann, J., Zinovoy, M., Greer, H., Yorke, E., Mageras, G., & Niethammer, M. (2021). Deep‐learning‐based image registration and automatic segmentation of organs‐at‐risk in cone‐beam CT scans from high‐dose radiation treatment of pancreatic cancer. Medical Physics, 48(6), 3084–3095. https://doi.org/10.1002/mp.14906 |
No other publications were recommended by dataset authors.
Research Community Publications
TCIA maintains a list of publications that leveraged this dataset. If you have a manuscript you’d like to add please contact TCIA’s Helpdesk.
Previous Versions
Version 1: Updated 2021/10/15
| Title | Data Type | Format | Access Points | License | Metadata | ||||
|---|---|---|---|---|---|---|---|---|---|
| Images and Radiation Therapy Structures | CT, RTSTRUCT | DICOM | Download requires NBIA Data Retriever |
40 | 40 | 240 | 16,962 | — |
